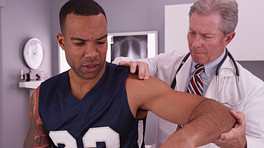
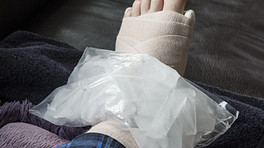
Once the location and severity of the athlete's stress fracture(s) is diagnosed, treatment can begin. Treatment protocols can range from simply a period of rest to casting, bracing, physical therapy, or even surgery, depending on the type and number of fractures, and/or the specific bone(s) affected.
In This Article:
- All About Stress Fractures
- Stress Fracture Causes
- Stress Fracture Symptoms
- Stress Fracture Risk Factors
- Stress Fracture Diagnosis
- Stress Fracture Treatment and Prevention
Rest. The first and often most important component of any stress fracture treatment program is to stop the activity that led to the stress fracture. 1 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures of the foot and ankle. July 2009: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=A00379. Accessed December 22, 2014. , 2 Martinez, JM. Stress fractures. May 23, 2013: Medscape. http://emedicine.medscape.com/article/1270244-overview. Accessed December 23, 2014. The rest period typically lasts 4 to 8 weeks, and may include simply switching to a lower-impact sport, such as changing from running to cycling or swimming. In some cases, patients may need to significantly decrease or even stop all physical activity altogether, depending on the type and severity of the fracture(s). 1 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures of the foot and ankle. July 2009: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=A00379. Accessed December 22, 2014. , 3 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures. October 2007: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=a00112. Accessed December 22, 2014.
Sometimes rest is all that is required to treat a stress fracture. (Unlike injuries that occur due to inflammation of tissue resulting from overuse, such as tendonitis, stress fractures do not respond to the “no pain no gain” exercise mentality.)
Protective footwear. Patients with stress fractures in their foot or ankle may need to wear special orthopedic footwear during the rest period to help reduce impact stress during the activities of daily living. 1 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures of the foot and ankle. July 2009: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=A00379. Accessed December 22, 2014. , 4 Wedro B. Stress fracture. eMedicineHealth.com. June 11, 2014: http://www.emedicinehealth.com/stress_fracture/article_em.htm. Accessed December 22, 2014. Examples of protective footwear include:
- Stiff-soled shoes or shoe inserts that prevent the flexing or bending of the foot
- A wood-soled therapeutic sandal
- A removable fracture brace that encases the foot and ankle
Casting and/or bracing. Some types of stress fractures take longer to heal and therefore require casting, such as those occurring on the outer side of the foot or in the ankle. In order to facilitate rest and aid the healing process, the use of casts, braces, or other immobilization devices may be used, either during the rest period, and/or after it. 1 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures of the foot and ankle. July 2009: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=A00379. Accessed December 22, 2014. Patients wearing casts and/or braces may require crutches or a wheelchair.
Common types of casts used to treat stress fractures include, but are not limited to: 2 Martinez, JM. Stress fractures. May 23, 2013: Medscape. http://emedicine.medscape.com/article/1270244-overview. Accessed December 23, 2014.
- Walking boots
- Pneumatic braces (air casts)
- Short plaster or fiberglass leg casts for stress fractures in the lower leg
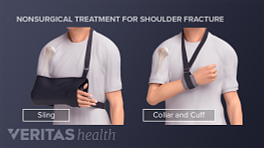
- Arm braces and/or slings for stress fractures of the upper or lower arm (commonly called little league shoulder or little league elbow), though this is uncommon
Physical therapy. After the initial rest and healing period ends, physical therapy is often recommended to help strengthen the affected bones, ease the return to athletic activity, and reduce the risk of re-injury. Common types of physical therapy include isometric strengthening exercises, water exercise, weight training, and stretching exercises. 1 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures of the foot and ankle. July 2009: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=A00379. Accessed December 22, 2014. , 5 Kishner S. Physical medicine and rehabilitation for stress fractures. January 27, 2014: Medscape. http://emedicine.medscape.com/article/309106-overview. Accessed December 22, 2014. , 8 Demetrious T, Harrop, B. Rib stress fracture. Physioadvisor. http://www.physioadvisor.com.au/14732250/rib-stress-fracture-physioadvisor.htm. Accessed December 23, 2014.
Surgery. In rare cases, surgery is required to correct stress fractures, especially severe and/or recurrent fractures in the feet and lower legs. Surgery to treat stress fractures often involves internal fixation, or the placement of metal pins, screws, and/or plates to help stabilize the affected bone(s) during and after the healing process. These methods are most commonly used in stress fractures of the feet if nonoperative treatments have failed to produce results.
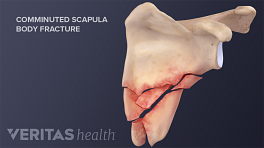
See Treating a Scapula Fracture
The most common long-bone stress fracture treated with surgery is a tibial stress fracture that compromises the structural integrity of the shin bone. This is often treated surgically with the implantation of an intramedullary rod that helps stabilize the tibia if conservative management has failed.
Upper extremity (arm) stress fractures are almost always successfully treated without surgery.
Stress fracture prevention
Stress fractures are often preventable if athletes adhere to appropriate training regimens and dietary habits. Common medical recommendations for reducing the risk of stress fracture include: 1 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures of the foot and ankle. July 2009: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=A00379. Accessed December 22, 2014. , 3 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures. October 2007: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=a00112. Accessed December 22, 2014. , 6 Beck, B. Stress fractures. American College of Sports Medicine, Current Comments. https://www.acsm.org/docs/current-comments/stressfractures.pdf. Accessed December 23, 2014.
- Wear appropriate footwear and other protective gear designed for each sport the athlete plays, and replace it often. Avoid playing sports in worn-out footwear and/or protective equipment.
- Increase exercise intensity gradually over a period of weeks or months to help the body adjust to each new level and reduce the risk of overuse injuries. Allow the same period of adjustment whenever changing sport(s) or playing surface, such as switching from sprinting to distance running, or from natural turf to artificial turf.
- Maintain proper nutrition, including dietary calcium and Vitamin D levels appropriate for the athlete's gender and age. Taking daily calcium and Vitamin D supplements in addition to eating a well-balanced diet rich in protein is recommended, especially for female athletes.
- Monitor the menstrual cycle (female athletes) and seek medical care if the menses become irregular or stop altogether, as this can be a warning sign of early-onset osteoporosis.
Athletes with stress fracture(s) or a history of stress fracture are advised to adhere to their doctors' treatment recommendations to prevent the injury from worsening and/or permanently affecting their athletic performance.
- 1 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures of the foot and ankle. July 2009: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=A00379. Accessed December 22, 2014.
- 2 Martinez, JM. Stress fractures. May 23, 2013: Medscape. http://emedicine.medscape.com/article/1270244-overview. Accessed December 23, 2014.
- 3 American Academy of Orthopedic Surgeons and the American Orthopedic Society for Sports Medicine. Stress fractures. October 2007: OrthoInfo. http://orthoinfo.aaos.org/topic.cfm?topic=a00112. Accessed December 22, 2014.
- 4 Wedro B. Stress fracture. eMedicineHealth.com. June 11, 2014: http://www.emedicinehealth.com/stress_fracture/article_em.htm. Accessed December 22, 2014.
- 5 Kishner S. Physical medicine and rehabilitation for stress fractures. January 27, 2014: Medscape. http://emedicine.medscape.com/article/309106-overview. Accessed December 22, 2014.
- 6 Beck, B. Stress fractures. American College of Sports Medicine, Current Comments.
- 8 Demetrious T, Harrop, B. Rib stress fracture. Physioadvisor. http://www.physioadvisor.com.au/14732250/rib-stress-fracture-physioadvisor.htm. Accessed December 23, 2014.