Hip flexor pain is often felt in the hip or groin and made worse by certain movements, such as kicking, pivoting at high speeds, or moving the knee towards the chest. The underlying cause of hip flexor pain may be:
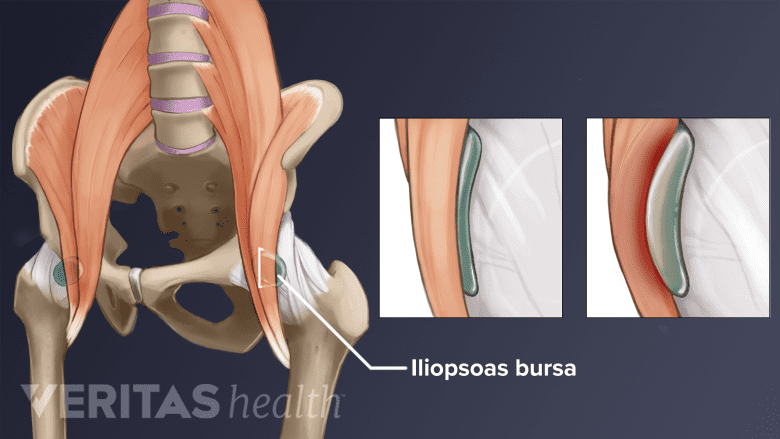
Injury to the iliopsoas bursa near the front of the hip joint is a cause of hip flexor pain.
In This Article:
- Understanding Hip Flexor Pain
- Causes of Hip Flexor Pain
- Video: Kneeling Hip Flexor Stretch
- Hip flexor strain or tear. A strain or tear refers to the damage caused to a muscle or tendon when it is stretched too far. Typically, a hip flexor strain or tear occurs when a person makes a sudden movement, such as changing direction while running. Muscle tears are classified on a grading system (mild to severe) that is determined by the severity of pain, loss of motion, and weakness in the affected area.
- Hip flexor tendinopathy. Tendons are the fibrous structures that attach muscle to bone. Hip flexor tendinopathy—which includes both tendonitis and tendinosis—may be caused by an acute injury, such as from a fall or car accident, or by overuse, such as from running, gymnastics, or soccer. Additionally, hip flexor tendinopathy can occur with age as the tendons naturally lose elasticity.
See What Is the Difference Between Tendonitis, Tendinosis, and Tendinopathy?
- Iliopsoas bursitis. Iliopsoas bursitis occurs when a hip’s iliopsoas bursa becomes inflamed. The iliopsoas bursa is a small, fluid-filled sac located between the front of the hip joint and the iliopsoas muscle. This injury is often seen in high-impact sports, such as soccer, skiing, or ballet. Iliopsoas bursitis can also be caused by arthritis.1Hip Bursitis. American Academy of Orthopedic Surgeons, OrthoInfo. https://orthoinfo.aaos.org/en/diseases--conditions/hip-bursitis/. January 2018. Accessed December 27th, 2018.
See Hip Bursitis on Arthritis-health.com
- Hip impingement. In most active adults, hip impingement is caused by abnormal bone growth and may cause a person to experience hip pain, usually in the groin area, and a decrease in the hip’s range of motion. There are 3 different types of hip impingement—cam, pincer, and combined. The type of hip impingement is determined by the location of abnormal bone growth.
See Pain Due to Hip Impingement (Femoroacetabular Impingement)
- Hip labral tear. The hip labrum is a ring of strong, flexible cartilage that rims the outer edge of the hip socket (acetabulum) and allows for a significant range of motion. When damaged, it may cause front hip or groin pain that is often described as a deep, dull, ache. Pain from a labral tear can appear gradually over time or suddenly. Labral tears are commonly seen in people who play sports that involve running, kicking, or turning.
- Osteoarthritis. Hip osteoarthritis is a common form of arthritis that occurs when the protective cartilage in the hip joint wears down over time. This cartilage normally reduces friction between the hip’s ball and socket during joint movement. Osteoarthritis may cause hip tenderness, stiffness, and a loss of flexibility.
See Hip Osteoarthritis Symptoms on Arthritis-health.com
- Overuse. Hip flexor pain can appear with no obvious underlying conditions or injuries. In these cases, the underlying cause may be overuse. People who frequently play sports that involve running, kicking, or turning, such as soccer or football, may experience pain from overuse.
- Pelvic obliquity (tilted pelvis). Medical professionals use the term pelvic obliquity to refer to a pelvis that is misaligned or tilted forward. Pelvic obliquity is associated with childbirth (in women), prolonged periods of sitting, lack of stretching, and poor posture. Pelvic obliquity may cause muscles in the hip or groin region to feel tight.
- Avascular necrosis (osteonecrosis). Very rarely, hip flexor pain is caused by avascular necrosis, a condition that occurs when blood supply to a bone is significantly reduced or completely cut off. Hip pain from avascular necrosis is often felt in the center of the groin, thigh, or buttocks and may develop gradually.2Osteonecrosis of the Hip. American Academy of Orthopedic Surgeons, OrthoInfo. https://orthoinfo.aaos.org/en/diseases--conditions/osteonecrosis-of-the-hip. January 2018. Accessed December 27th, 2018 Avascular necrosis is most often caused by trauma to the joint, such as a fracture or dislocation, but can also be from excessive steroid or alcohol use.
Some people may have more than one condition or injury that contributes to hip flexor pain. For example, it is possible to have both hip osteoarthritis and hip impingement.
Only a health care provider can accurately diagnose the cause of hip flexor pain. People who experience severe pain, pain that interrupts sleep or daily activities, or pain that lasts more than 2 weeks are encouraged to call or visit their health care provider.
Before getting a diagnosis, there are some at-home treatments that may reduce symptoms.
- 1 Hip Bursitis. American Academy of Orthopedic Surgeons, OrthoInfo. https://orthoinfo.aaos.org/en/diseases--conditions/hip-bursitis/. January 2018. Accessed December 27th, 2018.
- 2 Osteonecrosis of the Hip. American Academy of Orthopedic Surgeons, OrthoInfo. https://orthoinfo.aaos.org/en/diseases--conditions/osteonecrosis-of-the-hip. January 2018. Accessed December 27th, 2018

