Injuries to the hamstring muscles in the back of the thighs are extremely common on all levels of athletic competition.
They account for up to 29% of all lower extremity injuries across all sports and represent an important cause of back of the thigh and buttock pain.1Marshall S, Hamstra-Wright K, Dick R, Grove K, Agel J. Descriptive epidemiology of collegiate women's softball injuries: National Collegiate Athletic Association Injury Surveillance System, 1988-1989 through 2003-2004. J Athl Train 2007;42:286-94.,2Price R, Hawkins R, Hulse MH, A. The Football Association medical research programme: an audit of injuries in academy youth football. Br J Sports Med 2004;38:466-71.,3Shankar P, Fields S, Collins C, Dick R, Comstock R. Epidemiology of high school and collegiate football injuries in the United States, 2005-2006. Am J Sports Med 2007;35:1295-303.,4Marshall S, Covassin T, Dick R, Nassar L, Agel J. Descriptive epidemiology of collegiate women's gymnastics injuries: National Collegiate Athletic Association Injury Surveillance System, 1988-1989 through 2003-2004. J Athl Train 2007;42:234-40.,5Caine D, Nassar L. Gymnastics injuries. Med Sport Sci 2005;48:18-58.,6Woods C, Hawkins R, Maltby S, Hulse M, Thomas A, Hodson A. The Football Association Medical Research Programme: an audit of injuries in professional football--analysis of hamstring injuries. Br J Sports Med 2004;38:36-41.,7Orchard J, Marsden J, Lord S, Garlick D. Preseason hamstring muscle weakness associated with hamstring muscle injury in Australian footballers. Am J Sports Med 1997;25:81-5.,8Garrett W. Muscle strain injuries. Am J Sports Med 1996;24 S2-S8. For example, the incidence of hamstring injuries in the National Football League (NFL) was second only to knee sprains over a 10-year period.9Feeley B, Kennelly S, Barnes R, et al. Epidemiology of National Football League training camp injuries from 1998 to 2007. Am J Sports Med 2008;36:1597-603. Not surprisingly, the occurrence of hamstring injury in sports such as soccer, rugby, basketball, track and field, and gymnastics has been reported at a similar rate.4Marshall S, Covassin T, Dick R, Nassar L, Agel J. Descriptive epidemiology of collegiate women's gymnastics injuries: National Collegiate Athletic Association Injury Surveillance System, 1988-1989 through 2003-2004. J Athl Train 2007;42:234-40.,10Bennell K, Crossley K. Musculoskeletal injuries in track and field: incidence, distribution and risk factors. Aust J Sci Med Sport 1996;28:69-75.,11Hawkins R, Hulse M, Wilkinson C, Hodson A, Gibson M. The association football medical research programme: an audit of injuries in professional football. Br J Sports Med 2001;35:43-7.,12Orchard J, Seward H. Epidemiology of injuries in the Australian Football League, seasons 1997-2000. Br J Sports Med 2002;36:39-44.,13Brooks J, Fuller C, Kemp S, Reddin D. Incidence, risk, and prevention of hamstring muscle injuries in professional rugby union. Am J Sports Med 2006;34:1297-306.
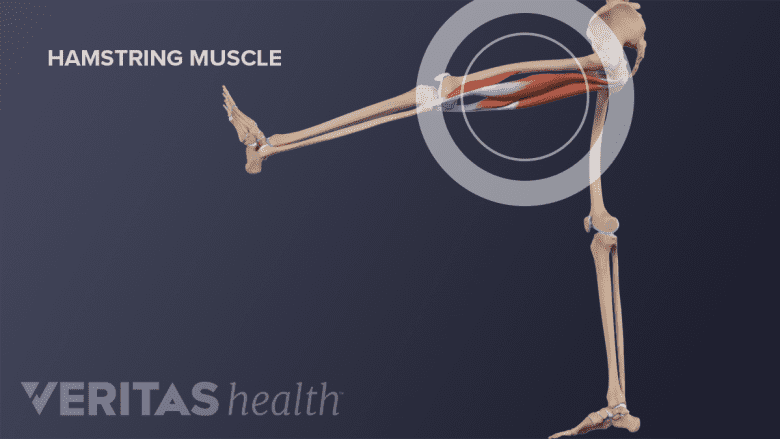
Hamstring muscle injuries are commonly seen in athletes.
In This Article:
An acute hamstring injury can commonly occur during exercise, but can also be the result of a fall or other accident. People with suspected hamstring injuries typically experience sudden pain at the back of the thigh with associated weakness, and are advised to seek medical attention.
Injury to the hamstrings can be detrimental with an average number of days lost to injury ranging from 8 to 25, depending on injury location and severity.9Feeley B, Kennelly S, Barnes R, et al. Epidemiology of National Football League training camp injuries from 1998 to 2007. Am J Sports Med 2008;36:1597-603.,13Brooks J, Fuller C, Kemp S, Reddin D. Incidence, risk, and prevention of hamstring muscle injuries in professional rugby union. Am J Sports Med 2006;34:1297-306. Unfortunately, there is a relatively high rate of re-injury, especially in the first two weeks following return to activity.2Price R, Hawkins R, Hulse MH, A. The Football Association medical research programme: an audit of injuries in academy youth football. Br J Sports Med 2004;38:466-71. Therefore, care must be taken to properly diagnose and treat an acute hamstring injury to avoid long-term complications, such as strength deficits and prolonged pain.
Why Are Early Diagnosis, Treatment, and Rehabilitation Important?
Getting an early diagnosis and receiving proper treatment for a hamstring injury is important because:
- Early recognition and appropriate management of hamstring injuries, followed by a proper return to activity, have been shown to result in improved functional outcome and prevention of future injuries.14Heiderscheit B, Sherry M, Silder A, Chumanov E, Thelen D. Hamstring strain injuries: recommendations for diagnosis, rehabilitation, and injury prevention. J Orthop Sports Phys Ther 2010;40:67-81.,15Askling C, Tengvar M, Tarassova O, Thorstensson A. Acute hamstring injuries in Swedish elite sprinters and jumpers: a prospective randomised controlled clinical trial comparing two rehabilitation protocols. Br J Sports Med 2014;48:532-9.,16Askling C, Saartok T, Thorstensson A. Type of acute hamstring strain affects flexibility, strength, and time to return to pre-injury level. Br J Sports Med 2006;40:40-4.,17Petersen J, Thorborg K, Nielsen M, Budtz-Jørgensen E, Hölmich P. Preventive effect of eccentric training on acute hamstring injuries in men's soccer: a cluster-randomized controlled trial. Am J Sports Med 2011;39:2296-303.,18Arnason A, Andersen T, Holme I, Engebretsen L, Bahr R. Prevention of hamstring strains in elite soccer: an intervention study. Scand J Med Sci Sports 2008;18:40-8.
- A re-injured hamstring typically takes longer to heal.2Price R, Hawkins R, Hulse MH, A. The Football Association medical research programme: an audit of injuries in academy youth football. Br J Sports Med 2004;38:466-71.,9Feeley B, Kennelly S, Barnes R, et al. Epidemiology of National Football League training camp injuries from 1998 to 2007. Am J Sports Med 2008;36:1597-603.,19Engebretsen A, Myklebust G, Holme I, Engebretsen L, Bahr R. Intrinsic risk factors for hamstring injuries among male soccer players: a prospective cohort study. Am J Sports Med 2010;38:1147-53.,20Gabbe B, Bennell K, Finch C, Wajswelner H, Orchard J. Predictors of hamstring injury at the elite level of Australian football. Scand J Med Sci Sports 2006;16:7-13., For example, it has been reported that NFL players with recurrent injuries needed 2.5 times longer for recovery and return to play than players with first-time injuries.9Feeley B, Kennelly S, Barnes R, et al. Epidemiology of National Football League training camp injuries from 1998 to 2007. Am J Sports Med 2008;36:1597-603.
- Hamstring injuries have been shown to result in permanent anatomical findings on MRI scans and in physical exams.
- High (proximal) hamstring injuries, if improperly managed, may eventually lead to a condition called chronic hamstring tendinopathy. This condition results in degeneration of the hamstring tendon, which connects the muscle to the ischial tuberosity (sit bone), and it can potentially cause significant pain and long-term disability. 21Lempainen L, Sarimo J, Mattila K, Vaittinen S, Orava S. Proximal hamstring tendinopathy: results of surgical management and histopathologic findings. Am J Sports Med 2009;37:727-34.,22Puranen J, Orava S. The hamstring syndrome--a new gluteal sciatica. Ann Chir Gynaecol 1991;80:212-4.,23Fredericson M, Moore W, Guillet M, Beaulieu C. High Hamstring Tendinopathy in Runners: Meeting the Challenges of Diagnosis, Treatment, and Rehabiliation. Phys Sports Med 2005;33:32-43.
This article will discuss the anatomy, mechanism of injury, risk factors, signs and symptoms, diagnosis, treatment, rehabilitation, and prevention of acute hamstring injuries.
Hamstring Muscle Anatomy
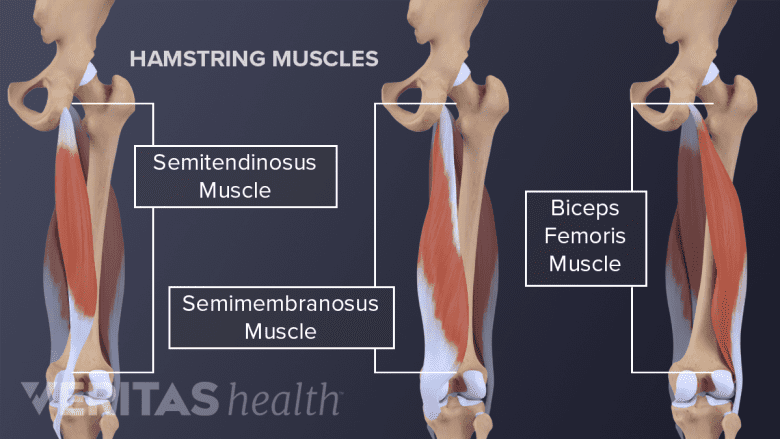
Hamstring muscles originate near the hip, travel down the back of the thigh, and end just below the knee joint.
What is commonly called the “hamstring” is actually a group of three muscles. These muscles originate near the hip, travel down the back of the thigh, and end just below the knee joint.
The three hamstring muscles include:
- The semitendinosus24Linklater J, Hamilton B, Carmichael J, Orchard J, Wood D. Hamstring injuries: Anatomy, Imaging, and Intervention. Semin Musculoskelt Radiol 2010;14:131-61.
- The semimembranosus
- The biceps femoris, which is the outermost muscle
The hamstrings have tendons at both ends for attachment to the hip and shin bones. Tendons are fibrous tissues that connect muscles to bones. Where the hamstring originates near the hip is called the proximal hamstring, and tendons connect the proximal hamstring to the bottom of the pelvis at the ischial tuberosity (or “sit bone”). Where the hamstring attaches past the knee joint is called the insertion.
All three hamstring muscles have insertions below the knee. Tendons of the semimembranosus and semitendinosus insert at the top of the tibia (shinbone). The biceps femoris tendon inserts at the top of the fibula, the long bone located outside of (lateral to) the tibia.
See Shin Splints (Medial Tibial Stress Syndrome)
The hamstrings have a higher proportion of type 2 muscle fibers when compared with other lower leg muscles. These type 2 muscle fibers, or fast twitch muscle fibers, enable hamstrings muscles to provide short, powerful contractions. The hamstring muscles contract while shortening (concentric contraction) during explosive take-offs and contract while lengthening (eccentric contraction) to help slow down the body during quick cutting moves and changes of direction.
Like all muscles in the body, activation of the hamstrings requires a nerve supply. The sciatic nerve (L5-S2 nerve roots), which runs down the back of the leg from the spine, provides nerves (innervation) to the hamstring muscles. Therefore, patients with sciatica may have pre-existing hamstring pain and weakness even prior to hamstring injury. Patients experiencing this type of pain should also be evaluated by a qualified medical professional.
- 1 Marshall S, Hamstra-Wright K, Dick R, Grove K, Agel J. Descriptive epidemiology of collegiate women's softball injuries: National Collegiate Athletic Association Injury Surveillance System, 1988-1989 through 2003-2004. J Athl Train 2007;42:286-94.
- 2 Price R, Hawkins R, Hulse MH, A. The Football Association medical research programme: an audit of injuries in academy youth football. Br J Sports Med 2004;38:466-71.
- 3 Shankar P, Fields S, Collins C, Dick R, Comstock R. Epidemiology of high school and collegiate football injuries in the United States, 2005-2006. Am J Sports Med 2007;35:1295-303.
- 4 Marshall S, Covassin T, Dick R, Nassar L, Agel J. Descriptive epidemiology of collegiate women's gymnastics injuries: National Collegiate Athletic Association Injury Surveillance System, 1988-1989 through 2003-2004. J Athl Train 2007;42:234-40.
- 5 Caine D, Nassar L. Gymnastics injuries. Med Sport Sci 2005;48:18-58.
- 6 Woods C, Hawkins R, Maltby S, Hulse M, Thomas A, Hodson A. The Football Association Medical Research Programme: an audit of injuries in professional football--analysis of hamstring injuries. Br J Sports Med 2004;38:36-41.
- 7 Orchard J, Marsden J, Lord S, Garlick D. Preseason hamstring muscle weakness associated with hamstring muscle injury in Australian footballers. Am J Sports Med 1997;25:81-5.
- 8 Garrett W. Muscle strain injuries. Am J Sports Med 1996;24 S2-S8.
- 9 Feeley B, Kennelly S, Barnes R, et al. Epidemiology of National Football League training camp injuries from 1998 to 2007. Am J Sports Med 2008;36:1597-603.
- 10 Bennell K, Crossley K. Musculoskeletal injuries in track and field: incidence, distribution and risk factors. Aust J Sci Med Sport 1996;28:69-75.
- 11 Hawkins R, Hulse M, Wilkinson C, Hodson A, Gibson M. The association football medical research programme: an audit of injuries in professional football. Br J Sports Med 2001;35:43-7.
- 12 Orchard J, Seward H. Epidemiology of injuries in the Australian Football League, seasons 1997-2000. Br J Sports Med 2002;36:39-44.
- 13 Brooks J, Fuller C, Kemp S, Reddin D. Incidence, risk, and prevention of hamstring muscle injuries in professional rugby union. Am J Sports Med 2006;34:1297-306.
- 14 Heiderscheit B, Sherry M, Silder A, Chumanov E, Thelen D. Hamstring strain injuries: recommendations for diagnosis, rehabilitation, and injury prevention. J Orthop Sports Phys Ther 2010;40:67-81.
- 15 Askling C, Tengvar M, Tarassova O, Thorstensson A. Acute hamstring injuries in Swedish elite sprinters and jumpers: a prospective randomised controlled clinical trial comparing two rehabilitation protocols. Br J Sports Med 2014;48:532-9.
- 16 Askling C, Saartok T, Thorstensson A. Type of acute hamstring strain affects flexibility, strength, and time to return to pre-injury level. Br J Sports Med 2006;40:40-4.
- 17 Petersen J, Thorborg K, Nielsen M, Budtz-Jørgensen E, Hölmich P. Preventive effect of eccentric training on acute hamstring injuries in men's soccer: a cluster-randomized controlled trial. Am J Sports Med 2011;39:2296-303.
- 18 Arnason A, Andersen T, Holme I, Engebretsen L, Bahr R. Prevention of hamstring strains in elite soccer: an intervention study. Scand J Med Sci Sports 2008;18:40-8.
- 19 Engebretsen A, Myklebust G, Holme I, Engebretsen L, Bahr R. Intrinsic risk factors for hamstring injuries among male soccer players: a prospective cohort study. Am J Sports Med 2010;38:1147-53.
- 20 Gabbe B, Bennell K, Finch C, Wajswelner H, Orchard J. Predictors of hamstring injury at the elite level of Australian football. Scand J Med Sci Sports 2006;16:7-13.
- 21 Lempainen L, Sarimo J, Mattila K, Vaittinen S, Orava S. Proximal hamstring tendinopathy: results of surgical management and histopathologic findings. Am J Sports Med 2009;37:727-34.
- 22 Puranen J, Orava S. The hamstring syndrome--a new gluteal sciatica. Ann Chir Gynaecol 1991;80:212-4.
- 23 Fredericson M, Moore W, Guillet M, Beaulieu C. High Hamstring Tendinopathy in Runners: Meeting the Challenges of Diagnosis, Treatment, and Rehabiliation. Phys Sports Med 2005;33:32-43.
- 24 Linklater J, Hamilton B, Carmichael J, Orchard J, Wood D. Hamstring injuries: Anatomy, Imaging, and Intervention. Semin Musculoskelt Radiol 2010;14:131-61.

