While extreme kneecap dislocations may be visible to the naked eye, doctors use a comprehensive diagnostic process to determine the presence and severity of a dislocated kneecap. This process will likely include a thorough discussion of the patient's medical history, as well as a physical examination and the use of diagnostic imaging techniques.
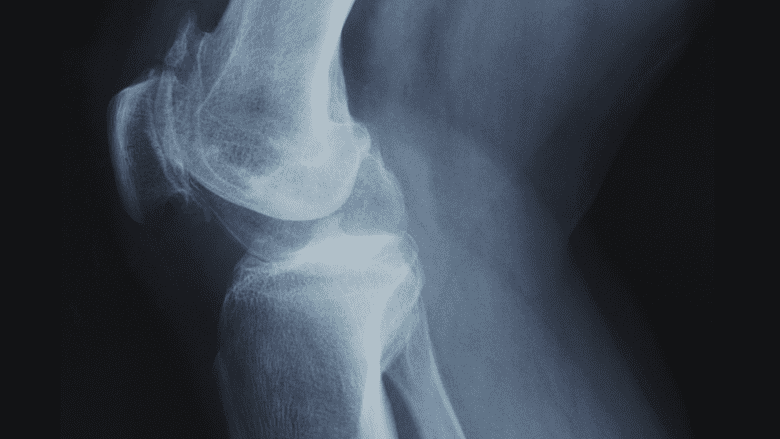
X-ray imaging may be used to diagnose a knee cap dislocation and determine the severity of the injury.
In This Article:
Patient History
In order to determine the likelihood that the injury is a kneecap dislocation, a doctor will ask some or all of the following questions:
- Have there been any knee injuries suffered in the past?
- Has this kneecap been dislocated before? How recently? How recently was treatment for that injury finished?
- Was the pain acute immediately following the injury? Did the pain only become noticeable over time?
- Is the pain throbbing, sharp, or aching? Where is the pain centralized? Does the pain worsen with touch?
- Is the pain constant or does it alleviate at all with rest?
- Is it possible to put any weight on the knee?
During the discussion of patient history, a physician will likely begin a physical examination. Conducting these two processes simultaneously will allow the doctor to ask relevant questions as physical signs of the injury present themselves.
Physical Examination
The examination will center on determining:
- Whether or not the kneecap has moved laterally to either the outside or inside of the leg.
- If swelling is present from internal damage.
- If bruising from physical trauma is present.
- Whether or not the athlete is able to extend the leg fully.
The physical examination will also be pivotal in determining whether or not other injuries were sustained at the time of the potential dislocation.
Imaging
Imaging will play a large role in diagnosing a kneecap dislocation, determining the severity of the injury, and developing a treatment plan. Two common imaging methods may be used:
- Magnetic Resonance Imaging (MRI). This type of imaging works by bouncing magnetic waves off of the affected area, generating an image of the tissues surrounding it. If a physician suspects that there may have been damage to a ligament, tendon, or cartilage within the knee during the dislocation, then an MRI will likely be used.
- X-Ray. This type of imaging allows a physician to gain a clear picture of the bone structure of the knee joint. In severe dislocations, the swelling may be so intense that the kneecap cannot be located without an X-Ray. An X-Ray can also be used to determine if there was any break or fracture sustained by the kneecap during the dislocation.

