Generally, surgery is a recommended option for people experiencing shoulder instability, pain, or stiffness after six months of undergoing nonsurgical treatment after a shoulder dislocation.

Bankart repair surgery reattaches the labrum to the shoulder socket.
Several surgeries can treat dislocated shoulders. The type of surgery is determined by several factors, such as the dislocation direction and possible soft tissue damage caused by the dislocation. It may be done as an open procedure or arthroscopically, using small incisions and instruments to guide the surgeon.
In This Article:
A Controversial Issue: Using Surgery Early in Treatment
Traditionally, nonsurgical treatment is tried before a surgical procedure for first-time shoulder dislocations and is not considered until the shoulder shows signs of chronic instability.
However, young people playing contact sports have an extremely high risk for a second dislocation after a first-time occurrence—up to 90% risk for recurrence.1Polyzois I, Dattani R, Gupta R, Levy O, Narvani AA. Traumatic First Time Shoulder Dislocation: Surgery vs Non-Operative Treatment. Arch Bone Jt Surg. 2016;4(2):104-8.
As a result, medical professionals are increasingly considering the possibility for young athletes with a first-time traumatic anterior shoulder dislocation to undergo surgery without attempting nonsurgical treatment first. A review of studies that included 239 active young men determined that surgical intervention resulted in significantly lower rates of dislocation recurrence, instability, or ongoing pain and stiffness.2Handoll HH, Almaiyah MA, Rangan A. Surgical versus non-surgical treatment for acute anterior shoulder dislocation. Cochrane Database Syst Rev. 2004;(1):CD004325.
Using surgery to treat a first-time shoulder dislocation has shown promise for young active males in particular, but has not been studied much for other populations groups and more research is needed. Currently, immediate surgery is not part of the standard treatment protocol.
Types of Surgery Used for Shoulder Dislocation
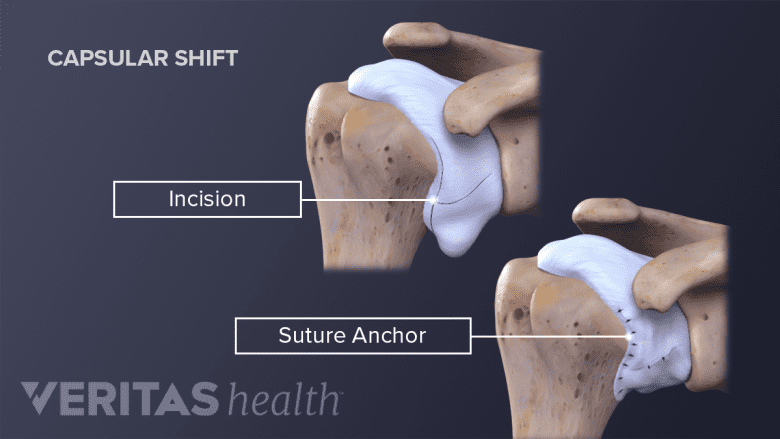
Capsular shift surgery tightens loose ligaments surrounding the shoulder.
These are the common procedures to treat shoulder dislocation:
- Capsular shift tightens the ligaments surrounding the shoulder that have stretched and loosened because of multiple dislocations. This procedure is usually done for people with natural (inherited) laxity, rather than people with traumatic injury. In general, patients who have conditions that predispose them to joint laxity, such as Elhers Danlos Syndrome, should approach the decision to have surgery with caution. There is a risk of needing repeat surgeries, which may make shoulder laxity worse overall.
- Bankart repair is commonly used for people with anterior dislocations, which is a dislocation toward the front of the body. Anterior dislocations can create a tear in the shoulder’s labrum, the cartilage around the shoulder’s socket. This kind of tear is known as a Bankart lesion. The torn labrum is repaired and re-anchored to the shoulder’s socket during a Bankart repair.
- Latarjet procedure may be recommended for a person with bone loss at the shoulder’s socket. A Latarjet procedure involves taking a small amount of bone material from the coracoid process (part of the shoulder blade) and transferring it to the front part of the shoulder’s socket. Bone loss in the socket can also be repaired with bone grafts taken from the patient’s iliac crest (part of the pelvic bone) or from a donor. Bone grafts from a donor or bone bank may increase the risk of infection.
- Remplissage procedure may also be needed if the shoulder’s ball, or humeral head, has been badly damaged by dislocation, causing a condition known as a Hill-Sachs lesion. The procedure involves resurfacing the head and/or filling in the defect by fixing it to part of the rotator cuff.
The recovery process for shoulder dislocation surgery can vary depending on what type of surgery was performed and what approach the surgeon used (open versus arthroscopic). Most people who have surgery wear a sling for several weeks and participate in physical therapy. A full recovery can take several months.
See Recovering from Shoulder Dislocation Surgery
Both open and arthroscopic procedures for shoulder dislocation have high success rates for improving function and preventing future dislocations.
See Physical Therapy and Recovery Timeline After Shoulder Dislocation Surgery
- 1 Polyzois I, Dattani R, Gupta R, Levy O, Narvani AA. Traumatic First Time Shoulder Dislocation: Surgery vs Non-Operative Treatment. Arch Bone Jt Surg. 2016;4(2):104-8.
- 2 Handoll HH, Almaiyah MA, Rangan A. Surgical versus non-surgical treatment for acute anterior shoulder dislocation. Cochrane Database Syst Rev. 2004;(1):CD004325.

