When a sports injury is unlikely to heal with traditional nonsurgical treatments, such as rest and physical therapy, a doctor may recommend a regenerative medicine treatment. This broad category includes treatments such as stem cell therapy, platelet rich plasma (PRP) therapy, prolotherapy, certain cartilage regeneration procedures, and more.
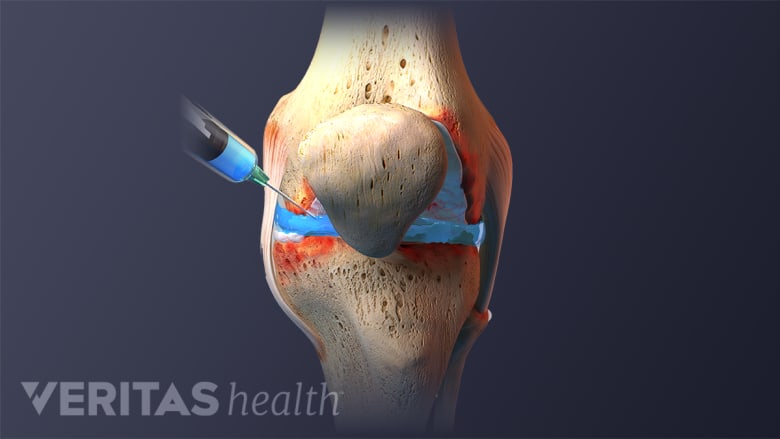
Regenerative medicine involves injecting a therapeutic solution into damaged tissue that will not adequately heal on its own.
In This Article:
- Regenerative Medicine for Sports Injuries
- Types of Regenerative Medicine for Sports Injuries
- Whether to Choose Regenerative Medicine Treatment
What Is Regenerative Medicine?
The National Institutes of Health defines regenerative medicine as “the process of creating living, functional tissues to repair or replace tissue or organ function lost due to age, disease, damage, or congenital defects.”1Regenerative Medicine. Last updated March 29, 2013. Accessed June 5, 2017. The hope is to restore damaged tissue that will not adequately heal on its own.
Regenerative medicine treatments can be divided into three categories:
Cellular therapies facilitate healing by injecting or placing live cells into the patient. Examples of cellular therapy include PRP and stem cell therapies, which can be used to treat tendinopathy and other sports injuries. Cellular therapy is sometimes called cell therapy or cytotherapy.
Read more about PRP Therapy and Stem Cell Therapy
- Tissue engineering replaces or repairs damaged tissue with natural tissue, man-made tissue, or a combination of both. In sports medicine, tissue engineering techniques may be used to treat cartilage injuries.
- Other therapies that attempt to trigger the body’s natural ability to heal tissues without introducing new cells or tissues. Prolotherapy is an example of this is type of therapy.
Four specific regenerative therapies are described on the next page.
How Is Regenerative Medicine Used for Sports Injuries?
In sports medicine, regenerative medicine treatments are typically used to repair or replace damaged cartilage, tendon, and ligament tissues.
Physicians who recommend regenerative medicine treatments for sports injuries hope to:
- Amplify the body’s natural healing abilities
- Encourage the growth of new tendons, ligaments, or cartilage tissue
The goal is to reduce pain and improve function.
Rest, physical therapy, bracing, and taping
Regenerative medicine is not a substitute for traditional nonsurgical treatments, such as rest, bracing, taping, and/or physical therapy to improve flexibility and strength. Regenerative medicine and traditional treatments can be used together to optimize healing.
Other applications for regenerative medicine
Regenerative medicine is not limited to treating sports injuries. For example, tissue engineering allows skin tissue to be created for burn victims. Other applications, such as developing artificial organs, are being researched.
Does Regenerative Medicine Work?
Clinical research studies of regenerative medicine treatments have shown mixed results but are generally encouraging. Most studies have been relatively small. More large-scale, high-quality clinical studies are needed before scientists can know exactly if and how regenerative medicine treatments help heal sports injuries such as tendinopathy.
See Does Stem Cell Therapy Work?
Interest in regenerative medicine has grown, particularly as some doctors and researchers look for a way to treat patients without NSAIDs or cortisone.2Malanga G, Nakamura R, Nakamurra R. The role of regenerative medicine in the treatment of sports injuries. Phys Med Rehabil Clin N Am. 2014;25(4):881-95. As time passes, individual doctors learn and share information, improving the application of these treatments.
See Are PRP Injections Effective?
Until more is known, regenerative medicine treatments are not considered standard practice and insurance plans typically do not cover them. Many patients are willing to pay out-of-pocket.

